September 28, 2016
℞ for the New York Region: How We Can Create a 'Culture of Health'
By Mandu Sen
When we talk about the wellbeing of a city or region, all too often we use economic data, such as income or employment statistics. Only rarely do we also take stock of our collective health. But there are many appropriate reasons why we ought to. Good health is, after all, the ultimate measure of a satisfying quality of life. At the same time, few factors more starkly or disturbingly map any locality’s social and political fault lines than do its racial, economic, and geographic disparities in health outcomes. And the full range of decisions that we collectively make about our natural and built environment – from the availability and quality of mass transportation to investments in affordable housing – directly and deeply affect the public health of an entire metropolitan area.
For these reasons, the Regional Plan Association (RPA) – a distinguished, nearly century-old urban research and advocacy organization – recently published a “State of the Region’s Health” report. We examine life expectancy statistics, prevalence of chronic illnesses, and other health indices and call for creating “a culture of health” in regional policy-making. In the coming year, the RPA will release the Fourth Regional Plan – a once-in-a-generation suggested blueprint for shaping the future of the New York metropolitan area. By deliberately incorporating health into how we plan our physical environment we can deliver better health outcomes, while expanding our economy and protecting our environment.
Here are the key facts from the “State of the Region’s Health”:
- Health care shapes only 20% of a community’s health in the U.S. Socioeconomic and environmental factors shape 80% of any community’s health.
- People in the region are living longer. In 1990, men’s life expectancy was 71, by 2010 it had increased to 78. In 1990, women’s life expectancy was 78, in 2010 it was 83.
- The region’s urban form, walkability, and connectivity can be a health advantage. For example, there are six deaths per 100,000 in the region due to motor vehicle crashes, a third of the national rate.
- There is room for improvement when it comes to quality of life. A typical adult reports 3.4 mentally bad health days & 3.5 physically bad health days per month in the region, higher than several comparable metros.
- There are also big disparities in health between different communities in the region. Life expectancy for blacks is 4-7 years shorter than for whites and Hispanics. Men in Morris County, New Jersey live six years longer than those in neighboring Essex County.
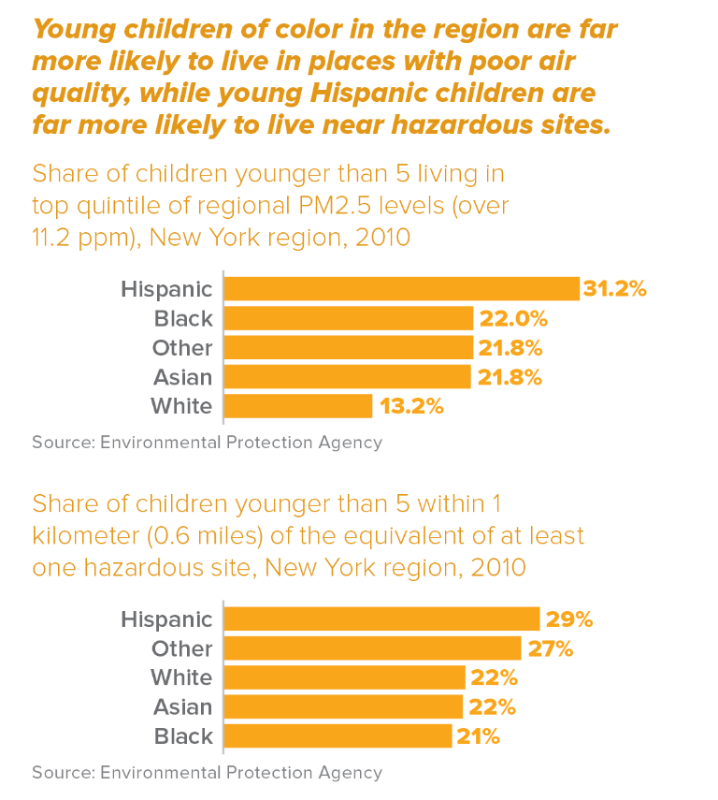
- Inequality and segregation contribute to health disparities. For example, Hispanic children are twice as likely to live in areas with high air pollution as white children.
- Health care costs have increased sharply in recent decades. Health care spending in Connecticut, New Jersey, and New York tripled between 1991 and 2009 from 92 billion to 259 billion dollars annually.
Here are selected figures from the report:
Note: PM 2.5 is the term for atmospheric particulate matter smaller in size than 2.5 microns – a fraction of the diameter of a human hair. Breathing air with high levels of PM2.5 pollutants can damage the health of young children, decrease lung function for people with asthma, and even increase the chance of heart disease amongst adults.
For the purposes of this analysis, hazardous sites include those are those that the Environmental Protection Agency defines as hazardous waste management facilities, Superfund sites, sites that require a chemical accident management plan, and point sources that discharge pollutants into waters of the United States.
Mandu Sen is a senior planner at the Regional Plan Association and the principal author of “State of the Region’s Health.”
Photo Credit: Jeffrey Swanson